I remember the first time I heard the term dense breasts.
I assumed it was just medical jargon and simply shrugged it off. Soon after, I learned that fibroglandular density (also referred to as breast density) plays a significant role in breast health.
But, what does it actually mean to have dense breasts? Does it affect your risk of breast cancer? Does it mean your mammography guidlines are different? How do you even know if you have high fibroglandular density?
To find out, we spoke with Dr. Elise Hotaling, a fellowship-trained breast imaging expert and Associate Professor at the University of Vermont.
Having a more dense breast composition (high fibroglandular density) makes it more challenging to detect cancer in a mammogram. If you would like an expert second opinion on your mammogram or other breast imaging scan from one of our subspecialty radiologists, you can learn more here.
[DocPanel] What is fibroglandular density? How does it affect a woman’s mammogram?
[Dr. Hotaling] Breast density refers to the relative amount of glandular and fibrous tissue (fibroglandular tissue) that each woman has in her breasts compared with the amount of fatty tissue present. Having a more dense breast composition (high fibroglandular density) makes it more challenging to detect cancer in a mammogram.
Let me explain why. Dense breasts appear more white on mammograms than non-dense breasts. But cancers usually appear white on mammograms, too. The more white the mammogram appears, the more difficult it is to detect cancer.
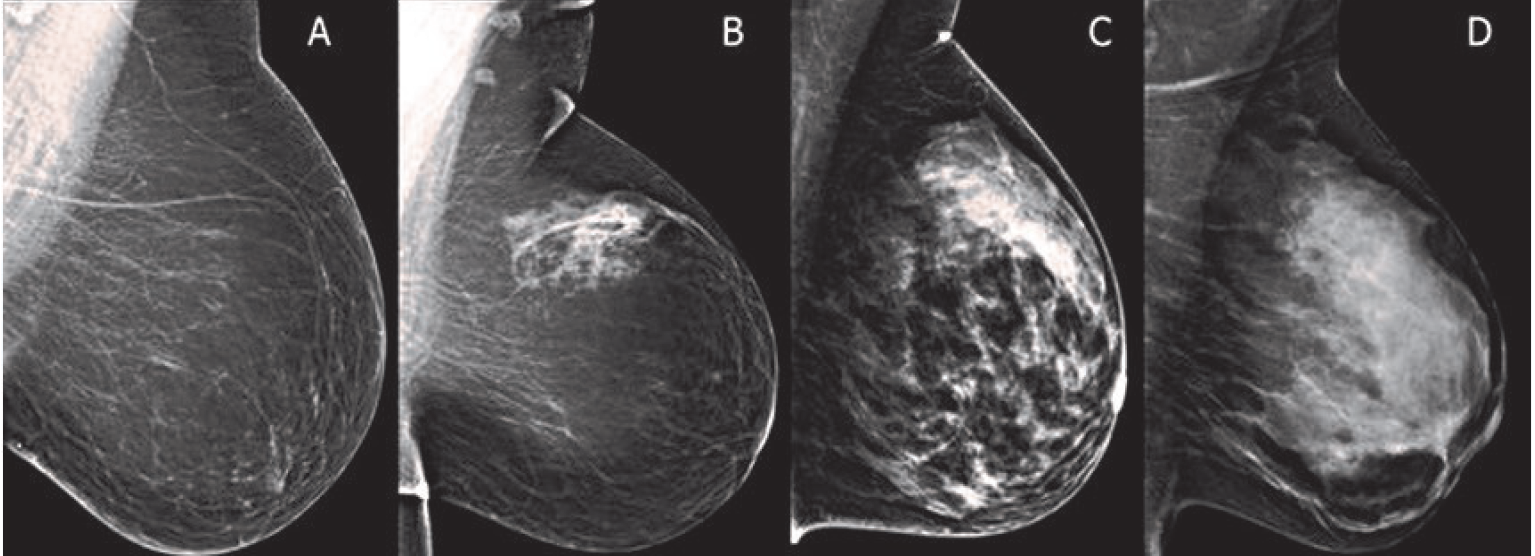
[Photo source: Cassling.com] Breast density from less dense (left) to higher density (right).
[DocPanel] What are the benefits of getting a second opinion on your mammogram or other breast imaging test?
If you have dense breast tissue, it is more challenging for radiologists to detect abnormalities on a mammogram. Having a radiologist who specializes in breast imaging review your scan can help make sure nothing was missed in the initial interpretation. Patients can also ask their second opinion radiologist whether additional imaging is recommended.
51% of breast cancer second opinions result in a changed diagnosis.
Second opinions are a powerful tool. It can confirm everything is fine, providing peace of mind and alleviating anxiety. Or, it may potentially prevent a missed cancer diagnosis. For patients with a breast cancer diagnosis, it can help ensure the cancer was accurately staged and confirm the best course of treatment is planned. It can also help prevent false positives.
Learn more about how to get a breast imaging second opinion here.
[DocPanel] How does fibroglandualr density affect a woman’s risk of getting breast cancer?
[Dr. Hotaling] 1 in 8 women will develop breast cancer at some point in their lifetime. The average woman’s risk is 12-13%.
Having a greater amount of fibroglandular tissue (a.k.a. dense breasts) slightly increases your risk. Family history, genetic mutations, prior radiation to the chest, beginning your period before age 12, and being female are other factors that also increase your risk.
[DocPanel] How can a woman know if she has dense breasts? Is it common?
[Dr. Hotaling] Dense breasts are normal. 40-50% of women have dense breasts. But there’s no way to measure fibroglandular tissue by touch or feel. It can only be determined through screening – not a physical exam.
[DocPanel] After a woman gets screened, will she be notified of her breast density?
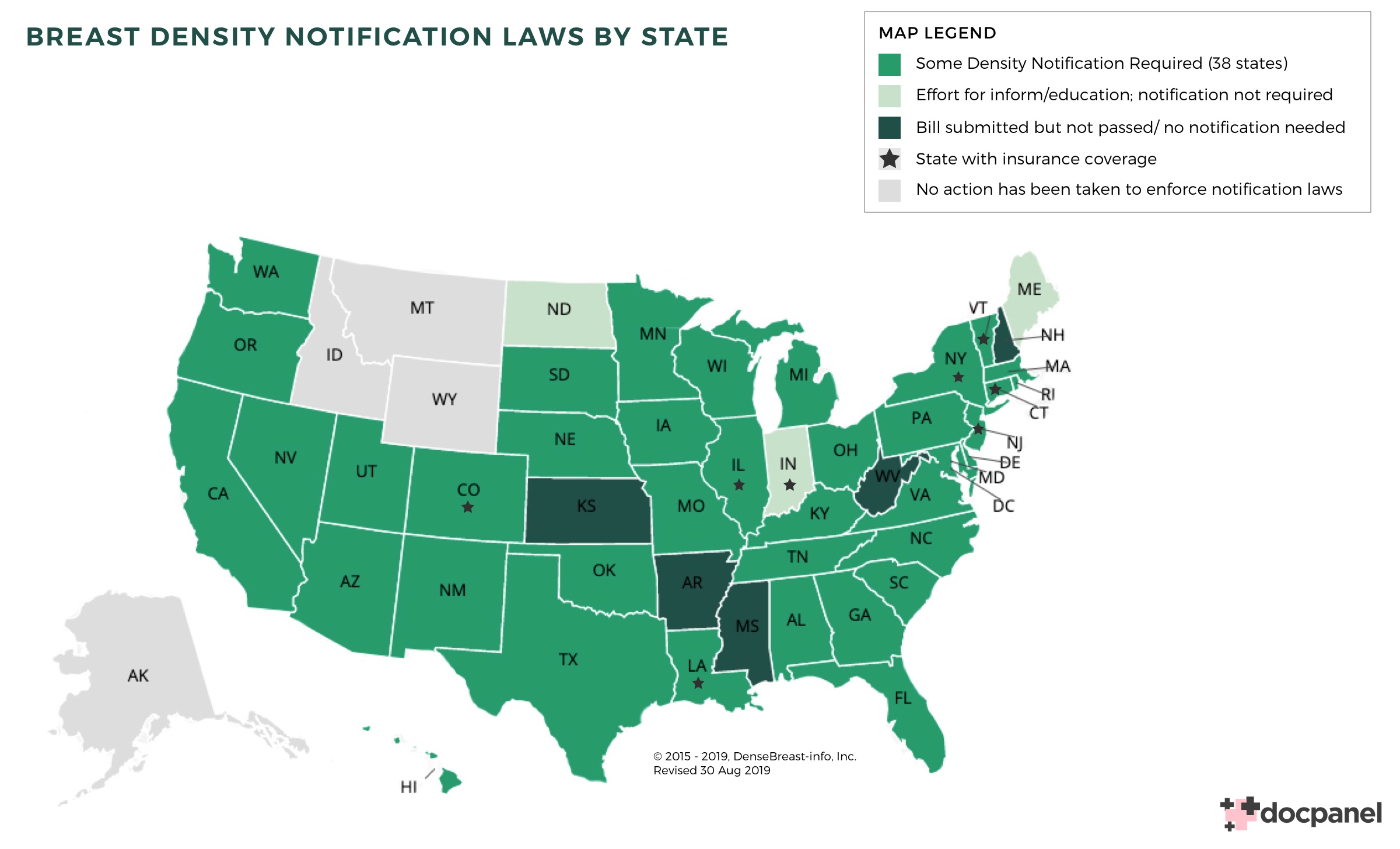
[Dr. Hotaling] In most cases, yes. Your mammogram report should include your breast density. Many states now have laws that require this. But there’s a small handful that do not.
Either way, breast density is a conversation every patient should have with their physician – preferably in person.
[DocPanel] Is high fibroglandualr density hereditary?
[Dr. Hotaling] It is at least partially inherited. If your mother has high fibroglandular tissue, it’s more likely you will too.
[DocPanel] Are there any other factors that influence breast density and the development of fibroglandular tissue?
[Dr. Hotaling] There are three other factors.
- Hormone therapy can increase both breast density and the risk of breast cancer.
- BMI – a measure of body fat based on weight and height – is also an independent risk factor for both breast density and breast cancer. Women with a low BMI are more likely to have high fibroglandular tissue. Before menopause, low BMI also increases the risk of breast cancer. After menopause, increased BMI and weight gain can potentially increase a woman’s risk of breast cancer.
- While there’s no exact correlation between fibroglandular tissue and breast size, smaller breasts tend to be denser (less fat). This is an important thing to note, as many women assume the opposite.
CONNECT WITH A SPECIALIST
Get a Second Opinion
Take charge of your health with an online second opinion from a radiology specialist.
[DocPanel] What BIRAD score would a woman with dense breasts most likely get? Will a mammogram that indicates dense breasts always result in a callback?
[Dr. Hotaling] Most likely, the patient would be BIRADS 1 (negative) or BIRADS 2 (benign).
Breasts with high fibroglandular density can also lead to more mammogram callbacks than fatty breasts – which will usually be indicated as a BIRADS 0 (need more images). In my practice, we include a statement that if your breast density is heterogeneous or extremely dense, an annual supplemental ultrasound may be considered in addition to annual mammography.
Learn more about the mamogram scoring system with our Practical Guide to Understanding BIRADS.
[DocPanel] If a woman has dense breasts, what questions should she be asking her referring provider?
[Dr. Hotaling] What is my lifetime risk of breast cancer? If you have dense breast tissue – does it fall in either the ‘heterogeneously’ or ‘extremely dense’ categories? If the answer is yes, you should consider getting a screening breast ultrasound in addition to mammography. And if your lifetime risk is over 20%, you should have an MRI to supplement your annual mammogram.
[DocPanel] What are the top three things you’d say to a woman with dense breasts?
[Dr. Hotaling]
- A physical exam cannot determine fibroglandualr density. It is only determined on a mammogram.
- I recommend that all women consider 3D mammography. 3D mammography improves cancer detection in all breast densities – especially for women with high (heterogeneously) fibroglandular density. 3D Mammography has a lower false-positive rate than 2D mammograms. They also decrease the callback rate. You can speak with your healthcare provider to request one. Not all insurance plans cover them, but depending on a woman’s risk, she may qualify to have a 3D mammogram instead of a 2D exam.
- Discuss your breast density and risk factors with your doctor. This will help determine which screening tests may be right for you. Supplemental breast screening ultrasound or MRI may be indicated based on each individual’s risk factors and values.
[DocPanel] What is the one thing you’d like to see happen soon regarding breast density? How do you think it can be achieved?
[Dr. Hotaling] I would like women to understand what breast density means, and to have the necessary information to make an informed decision about their screening options. Each patient should have the opportunity to discuss their values and preferences with their healthcare provider.
By informing women of their breast density and providing education on what fibroglandular tissue actually means – physicians can help personalize a woman’s health care. Breast density and breast cancer risk are unique to each and every woman. The recommended test(s) suggested for one woman with dense breast may differ vastly from that of another woman with more fatty breast tissue.
If you have questions or concerns about the density of your breasts, or in regards to the best screening for your particular body, always consult a healthcare provider.
This article features an interview with Dr. Elise Hotaling. Get your scans interpreted by one of the nation’s leading subspecialists. Request a second opinion today.

