Getting a mammogram callback can trigger anxiety in just about any woman.
But out of all women called back after an inconclusive mammogram, less than 0.5% will have cancer.
"A callback is a pretty generic term we use. It doesn’t mean you have cancer. It just means come back, we need some more information," says Dr. Cindy Lee. "Getting additional imaging (referred to as a diagnostic mammogram) is important, but it doesn’t have to be a scary experience."
We sat down with Dr. Lee, expert breast imager and Assistant Professor of Radiology at a major academic center in New York, to debunk myths about the mammogram callback.
In this interview, we explore what a diagnostic mammogram is, why they matter, and what the liklihood is of a mammogram callback resulting in a negative finding.
To learn the ins and outs of understanding mammogram callback reasons, how the process works, and what we as women should be asking our physicians – visit part two of our Mammogram Callbacks Series.
Understanding Your Diagnostic Mammogram
[DocPanel] What is a mammogram callback?
[Dr. Lee] After a routine screening mammogram, we may call a patient back for additional images – reffered to as a diagnositc mammogram – to clarify any findings.
Especially for women who are getting their breasts screened for the first time, inconclusive mammograms are quite frequent. Since there are no prior images to compare the pictures to, your radiologist might want to get a few more views to be sure everything is fine.
[DocPanel] Why is it important to pay attention to a callback?
[Dr. Lee] A callback means the mammogram is indeterminate or abnormal, and there are areas in the breast that your doctor needs to evaluate further. While most callbacks end up being normal, the diagnostic mammogram follow-up is still very important. The additional imaging may influence your screening plan going forward, or it may identify an area that needs to be closely monitored as a precaution. In the rare case that there is cancer, your diagnostic mammogram could save your life.
If for some reason you are unable to go back in for your callback (maybe you’re traveling, etc.) – you can get an online second opinion from a breast imaging specialist through DocPanel. You can then ask the radiologist whether or not they think you should get further imaging. They might be able to reassure you that everything is fine without you having to get further testing – or, they may agree and advise the same.
Regardless of whether or not you get more scans – a second opinion is always a wise choice. Breast abnormalities are difficult to detect when small – it absolutely helps to have multiple eyes read your scans.
[DocPanel] How will a patient be notified that they’re being called back?
[Dr. Lee] By law, every patient who had a mammogram test is required to get a letter with their results within 30 days. That’s a federal law. But sometimes, even before they receive the letter, a patient may get a call from their physician or doctor’s office, notifying them that they need a diagnositc mammogram.
[DocPanel] Does the timing or method of callback notifications change based on the mammogram callback reason?
[Dr. Lee] No, all callbacks follow the same process, so the timing is relatively similar. It’s your radiologist’s request for more information with a dignostic mammogram and/or diagnostic ultrasound.
[DocPanel] How long will a patient have to wait for their diagnostic mammogram results?
[Dr. Lee] When a patient returns for a diagnostic mammogram or ultrasound, a radiologist will read the images in real-time. So everyone will receive their results before they leave the office. The results can be normal (BI-RAds 1 or 2), can require a short term follow up (BI-RADS 3), or may require a biopsy (BI-RADS 4 or 5). BI-RADS 0 means additional images are needed and is only used to callback screened patients who require a diagnostic mammogram.
Learn more about the mammogram scoring system in our Practical Guide to Understanding BIRADS.
Mammogram Callback Prevalence
[DocPanel] What percentage of callbacks result in an abnormal finding? What advice do you have to help women manage the stress and anxiety that a diagnostic mammogram might trigger?
[Dr. Lee] Most diagnostic mammograms will be normal.
Only about 10% of our patients are called back. But there’s a lot of anxiety attached to the word ‘abnormal.’ So in their heads, everyone is thinking, "oh my god, I have cancer."
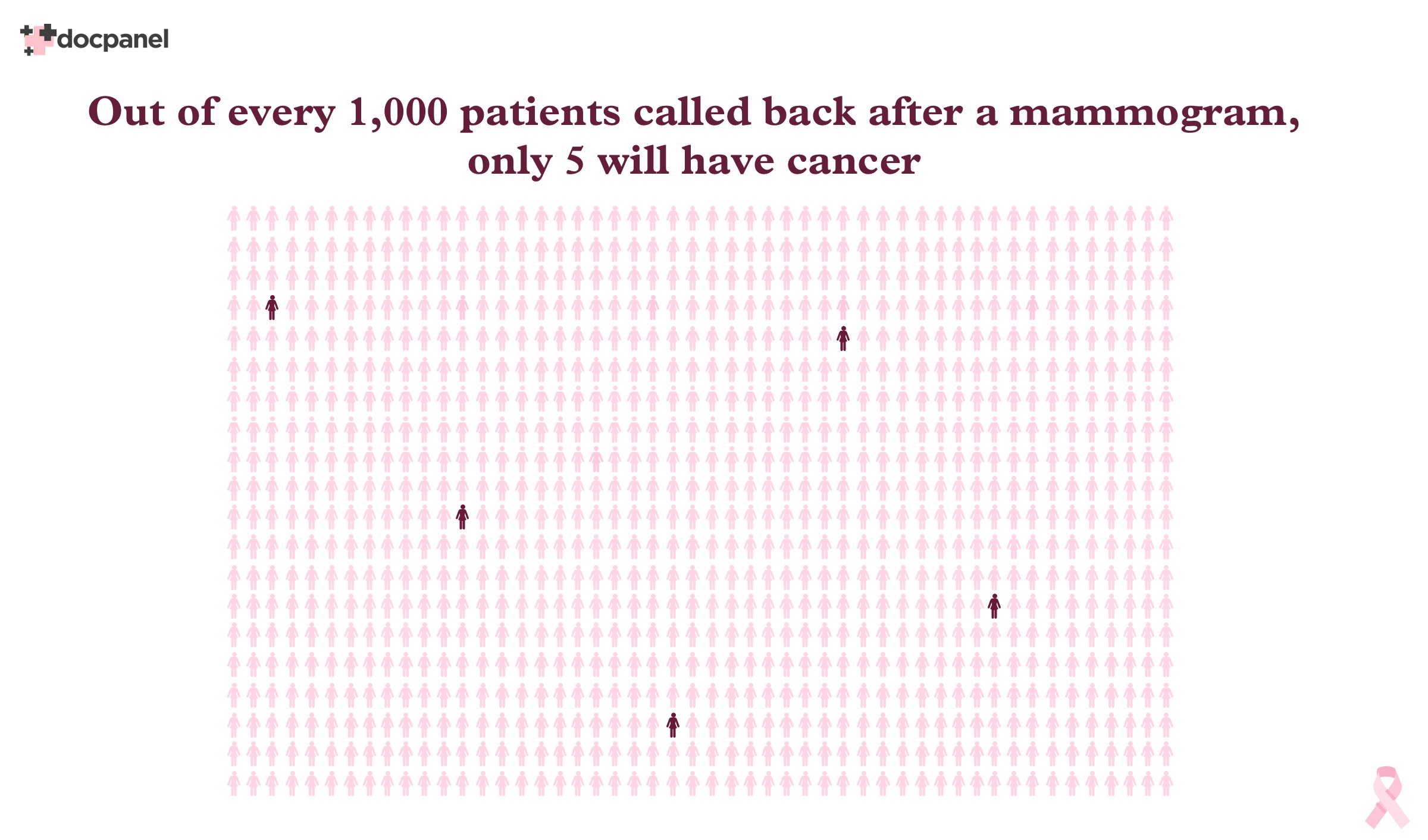
But that’s not the case at all. Only 10-20% will need a biopsy, and out of the biopsy group, only about one third will have cancer. So you’re looking at somewhere around 5 patients per 1,000 that will have cancer. It’s really low.
My advice is for women is to just make sure they go back as soon as possible. Because the relief comes when I tell them everything on their dignostic mammogram is normal – and that’s most often the case. When I give them the negative result and say everything we did today was perfect, you’re good for the year – the anxiety will disappear. The sooner a patient returns for their callback, the better. If you don’t come back, that anxiety can linger.
[DocPanel] When reading a mammogram report, what other terms indicate a callback is required?
[Dr. Lee] We provide a BI-RADS Score for all breast ultrasounds, mammograms, and breast MRIs. A BI-RADS score is a breast imaging interpretation score.
This makes it simple for people to know – is this something I have to worry about? Is there anything there? What do I do next?
In addition to a BIRADS score, mammogram reports will also have the word ‘abnormal’ or ‘normal’ (although the verbiage for this may differ slightly from clinic to clinic).
If a woman’s screening mammogram is normal, she will get either a BIRADS 1 or 2, which means everything is normal this year… we’ll see you next year, don’t worry. If she has an inconclusive mammogram that requires a callback – she will get a BIRADS 0, and her report will say ‘abnormal.’ But all a BI-RADS 0 means is that additional images (a diagnostic mammogram) are needed.
Most of the time, all ‘abnormal’ means is that more information is needed. It very rarely indicates that there’s an actual cancer finding.
[DocPanel] Is there anything that can be done to help decrease the frequency of callbacks?
[Dr. Lee] Yes, 3D mammograms. 3D technology is just so much better. You don’t have to call as many people back, and you also catch more cancer with it. When available, it’s the preferred modality.
At NYU, which is where I work, we’re 99% 3D. New York, as a whole, is fantastic in that nearly everyone has 3D machines. But that’s not true for the rest of the country. Depending on where the patient is, they may only have access to a 2D mammogram machine. In that case, alternate imaging modalities may only be available post a callback, if a radiologist feels the patient needs one.
When it comes to breats imaging, Dr. Lee reminds us that we shouldn’t have to feel nervous or confused. Whether it be additional imaging, a second opinion, or a call to your doctor, information is always within reach.
Next, find out how one woman navigated her way from fear to peace of mind after an abnormal mammogram in our patient feature story: How a Second Opinion Helped Me Understand My Abnormal Mammogram.

Why Get a Breast Imaging Second Opinion
51% of breast cancer second opinions result in a changed diagnosis.
A second opinion from a breast imaging subspecialist is valuable for both patients with and without a breast cancer diagnosis.
For those without a diagnosis, it can offer peace of mind and confirmation that nothing was missed. Or, it could potentially prevent a missed cancer diagnosis. For patients with a breast cancer diagnosis, it can help ensure the cancer was accurately staged and confirm the best course of treatment is planned. It can also help prevent false positives.
Get your scans interpreted by one of the nation’s leading subspecialists. Request a second opinion today.
