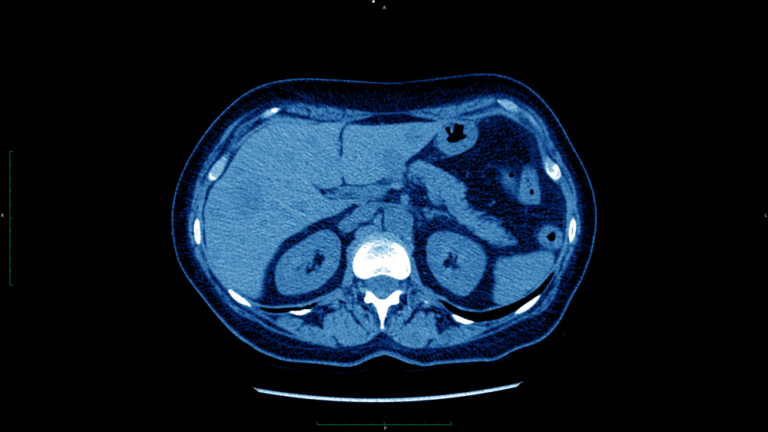
What Are Focal Nodular Hyperplasia Liver Lesions
Focal nodular hyperplasia liver lesions, also called FNH, are tumors characterized by the presence of a vascular mass with nodules. They usually develop in singular form but can appear as multiples in rare cases.
DocPanel is committed to making sure every patient receives excellent care. If you would like an expert second opinion on a liver lesion diagnosis from one of our subspecialty radiologists, you can learn more here.
How Common Are Focal Nodular Hyperplasia Liver Lesions
Focal nodular hyperplasia liver lesions are the second most common benign liver lesion. The majority of cases are found in premenopausal women between the ages of 20 and 50 years, with about 10 to 20 percent of all cases occurring in men. Some believe prolonged use of oral contraceptive pills may possibly contribute to the development of FNH liver lesions; however, there is a considerable amount of debate in regard to this claim.
Focal nodular hyperplasia liver lesions are usually asymptomatic, rarely grow or bleed, and do not present the risk of malignant transformation. However, differentiating focal nodular hyperplasia liver lesions from other liver tumors can be very difficult. Risk of misdiagnosis is high with FNH liver lesions. They are most commonly mistaken as hepatic adenoma liver lesions or intrahepatic cholangiocarcinoma. An accurate diagnosis is critical to avoid unnecessary biopsy, surgery, or other invasive treatment methods. An experienced subspecialty radiologist is the best way to ensure an accurate diagnosis.
How Are Focal Nodular Hyperplasia Liver Lesions Detected
In most patients, focal nodular hyperplasia liver lesions are incidentally discovered during cross-sectional imaging. While FNH liver lesions are not necessarily an issue – they are often mistaken for other liver lesions, drastically impacting the next steps in patient management.
Focal nodular hyperplasia liver lesions can display similar characteristics found in hepatic adenoma liver lesions and intrahepatic cholangiocarcinoma. It also shares imaging features with the fibrolamellar variant of hepatocellular carcinoma. The risk of FNH being misdiagnosed as liver cancer is high, meaning it is essential images be interpreted by a specialist. A second opinion is also recommended to confirm diagnosis and avoid unnecessary biopsy, surgery, or other invasive treatment methods.
MRI tends to be more sensitive to identifying and picking up FNH specific characteristics than CT. Doppler ultrasonography and contrast enhanced ultrasonography have been shown to further improve the accuracy of FNH liver lesion diagnosis. Inconclusive cases may require biopsy or surgical resection; however, these are best avoided.
Focal Nodular Hyperplasia Liver Lesion Symptoms
Most focal nodular hyperplasia liver lesions are asymptomatic. Some patients, however, may experience abdominal pain and mild GI discomfort.
Focal Nodular Hyperplasia Treatment
Focal nodular hyperplasia liver lesions are typically left untreated. Unlike hepatic adenoma liver lesions, they do not pose a threat of rupture.
Patients with suspicious liver lesions should keep in mind the diagnostic challenge in accurately identifying focal nodular hyperplasia liver lesions. Given their tendency to be misdiagnosed, FNH cases run the risk of mistreatment. A second opinion can help ensure accurate treatment planning and management.
Risk Factors
There is some belief that oral contraceptive pills may contribute to the development of focal nodular hyperplasia liver lesions. However, there is currently minimal evidence to support this correlation. Some physicians recommend that patients diagnosed with FNH lesions should discontinue use of OCPs.
Get a Subspecialty Second Opinion Today
The DocPanel platform enables people all over the world to get an expert second opinion in as little as 24 – 72 hours.
An easy 3-step process – instantly upload your scans, select an expert subspecialty radiologist (or have DocPanel assign your case to the appropriate subspecialist), and submit your request. Upon uploading your scans, you’ll also have the opportunity to ask any questions you might have about your case.
Not sure what a subspecialist is? Learn more with our in-depth article on the importance of getting a second opinion from a subspecialty radiologist.
Dr. Richard Semelka, leading expert in abdominal imaging, has been practicing radiology for over 28 years. He’s written over 16 text-books, 370 peer-reviewed papers, and has over 21,000 research citations in Abdominal Imaging.
Get your scans interpreted by Dr. Semelka or explore DocPanel’s complete team of subspecialty radiologists. Request a second opinion today.