What Are Liver Lesions
Liver lesions are groups of abnormal cells or tissues. Also referred to as a liver mass or tumor, liver lesions can be either benign (noncancerous) or malignant (cancerous). Benign liver lesions are very common and are generally not a cause for concern. Malignant liver lesions, however, require intervention and treatment.
DocPanel is committed to making sure every patient receives excellent care. If you would like an expert second opinion on a liver lesion diagnosis from one of our subspecialty radiologists, you can learn more here.
How Are Liver Lesions Found
Liver lesions are detected through radiographic imaging, such as an ultrasound, CT, or MRI. Generally speaking, MRI is the preffered method for evaluation given its capabilty to image soft tissue.
Ensuring an Accurate Liver Lesion Diagnosis
Once a liver lesion is detected, a radiologist will need to identify the type and nature of the lesion (cancerous vs noncancerous). This is extremely important, as the correct treatment and management approach varies greatly from one kind of liver lesion to the next.
But liver lesions are very complex. Malignant liver lesions share characteristics with benign liver lesions, some benign lesions can be left alone while others require surgery, and certain types of benign lesions have the propensity to develop into cancer.
23% OF PATIENTS DIAGNOSED WITH LIVER CANCER DON’T ACTUALLY HAVE CANCER AT ALL
Patients misdiagnosed with liver cancer may receive debilitating treatments that are unnecessary and expensive, while cancerous liver lesions misjudged for benign lesions will have the opportunity to grow and advance into late stage cancer.
With so many diagnostic pitfalls, liver lesion cases fall outside of a general radiologist’s scope. The ability to correctly identify a mass requires familiarity that comes from specific training and years of practice. Getting your scans read by an abdominal subspecialty radiologist can help ensure accuracy and prevent misdiagnosis. Through DocPanel, you can submit your scans online and have a subspecialty radiologist review them and provide a second opinion. It’s a quick, easy, and much more affordable way to get the same level of care as you would if you were to take your scans to a prestigious hospital.
Benefits of a Liver Lesion Second Opinion
Familiarity in distinguishing different types of liver lesions from one another takes years of experience and specialized training. Liver lesion identification is especially complex because different types of lesions share simialr characterisitics with one another.
Getting a second opinion from an abdominal radiology subspecialist helps ensure:
- that the liver lesion is correctly identified
- that cancer, if present, is accurately staged
- that the option for surgical resection is properly evaluated
- that the patient has an opportunity to voice their questions and concerns
- that the patient is aware of all their treatment options
Liver Lesion Symptoms
Most liver lesions are asymptomatic. Even cancerous (malignant) tumors do not generally present any symptoms in the early stages. As a result, many liver lesions are discovered incidentally during imaging studies for unrelated conditions.
Because there usually are not any symptoms that help let doctors know what type of liver lesion a patient has, it’s all left up to image interpretation. In order to ensure accuracy, image interpretation by a subspecialty radiologist with extensive expertise in identifying masses of the abdomen is crucial.
Types of Liver Lesions
Benign Liver Lesions
Benign liver lesions are found in more than 20% of the general population. They make up the majority of all liver lesions in the United States and can usually be left untreated. They do not spread to other parts of the body, and typically do not pose a serious threat. However, if liver lesions cause pain, grow too large, are at risk of rupture, or cause internal bleeding, they may need to be surgically removed.
Hemangioma Liver Lesions
The most common type of benign liver lesion, a liver hemangioma is an abnormal mass of blood vessels. Found in around 5 percent of adults, they are asymptomatic and typically go undiscovered. They do not pose a threat themselves; however, they can easily be mistaken for other malignant lesions in radiographic images. In order to prevent misdiagnosis, it is imperative suspicious scans are interpreted by a subspecialty radiologist with extensive experience in abdominal imaging.
Learn more about hemangioma liver lesions.
Hepatic Adenoma Liver Lesions
Hepatic adenoma lesions are uncommon benign liver lesions, with an estimated incidence of 3 – 4 per 100,000 women. They are typically found in women who regularly use oral contraceptive pills, or in athletes taking anabolic steroids. Some hepatic adenoma lesions have a high potential for malignant progression, spontaneous hemorrhage, and rupture. Differentiating them from other liver lesions is imperative for appropriate patient management. A hepatic adenoma can be detected with radiographic imaging, but distinguishing them from other lesions is difficult and requires a specialty radiologist.
Learn more about hepatic adenoma liver lesions.
Focal Nodular Hyperplasia Liver Lesions
Focal nodular hyperplasia liver lesions, also called FNH, are the second most common solid benign liver lesion. FNH liver lesions are usually asymptomatic; however, some patients may experience abdominal pain and mild GI discomfort. While focal nodular hyperplasia lesions are not threatening, differentiating them from other liver tumors can be very difficult. Because of this, there is a high risk of misdiagnosis. Focal nodular hyperplasia lesions share imaging features with the fibrolamellar variant of hepatocellular carcinoma. They also display similar characteristics found in hepatic adenomas. Proper diagnosis is critical to avoid unnecessary biopsy, surgery, or other invasive treatment methods. To ensure an accurate diagnosis, it is highly advised patients get several complementary imaging scans, and that the images be interpreted by an experienced subspecialty radiologist.
Learn more about focal nodular hyperplasia liver lesions.
Other Benign Liver Lesions Include:
- Liver Cysts
- Biliary hamartomas
- Lipomas
Malignant Liver Lesions
Each year approximately 21,000 men and 8,000 women get liver cancer in the United States, and about 16,000 men and 8,000 women die from the disease. Malignant liver lesions can be classified into two types of liver cancer: primary liver cancer and secondary liver cancer.
Primary liver cancer, also called hepatoma and hepatocellular carcinoma, is a cancer that starts in the liver. Secondary liver cancer, also referred to as liver metastases, is a cancer that spreads to the liver from another organ. In the US, secondary liver cancer is 18-40 times more common than hepatoma. Cancerous liver lesions are life threatening. They require intervention and meticulous follow-up management after a diagnosis.
Hepatoma (Hepatocellular Carcinoma Liver Lesions)
The most common type of primary malignant liver lesion is hepatoma (hepatocellular carcinoma). It is most commonly associated with cirrhosis – a late stage of liver damage caused by various diseases and conditions, but usually linked to chronic alcoholism or hepatitis B or C infection.
The fifth most common cancer in the world, and the third most common cause of cancer-related death, early detection is crucial for successful treatment. But identifying hepatocellular carcinoma liver lesions can be difficult, as they have a variety of appearances in imaging and can easily be mistaken for benign liver lesions. A second opinion from a subspecialist radiologist is strongly encouraged to confirm a diagnosis.
Learn more with our post on how to navigate a liver cancer diagnosis.
Liver Metastases (Hepatic Metastases)
Also called secondary liver cancer, liver metastases develop when cancer from another part of the body spreads to the liver. Benign liver lesions share numerous characteristics with hepatic metastases. Hemangiomas and focal nodular hyperplasia (FNH) are particularly difficult to differentiate from metastatic disease and are a serious cause of confusion during image interpretation. A thorough understanding of the various appearances of hepatic metastases is crucial for accurate diagnoses. For patients undergoing treatment for hepatic metastases, follow-up imaging is a crucial component of patient management.
Learn more about liver metastases.
Other Malignant Liver Lesions Include:
- Intrahepatic cholangiocarcinoma (bile duct cancer
- Hepatoblastoma
- Angiosarcoma (also called hemangiocarcinoma)
What Causes Liver Lesions
Most benign liver lesions are not linked to a direct cause. They can be found on anyone and, most often, do not pose a threat. The majority of malignant liver lesions are a result of cancer that spreads to the liver from another organ. Primary malignant liver lesions – meaning cancer cells that originated in the liver – are most commonly associated with cirrhosis, caused by heavy alcohol consumption, hepatitis B infection, or hepatitis C infection. Although usually a benign condition, those with advanced fatty liver disease run the risk of developing cirrhosis, which can lead to liver cancer.
Detecting Liver Lesions
Liver lesions can be diagnosed using a combination of blood tests and imaging tests. Each modality has its own advantages and disadvantages when it comes to characterizing liver tumors. Depending on the type of liver lesion suspected, appropriate scans will be used in conjunction with one another to determine a diagnosis. In inconclusive cases, a biopsy may be required to determine malignancy; however, most physicians prefer to avoid such procedures due to their invasive nature.
Liver Lesions on Ultrasound
Most liver lesions are initially detected during an ultrasound. It is highly sensitive at differentiating a cyst from a solid liver lesion and serves as a good first step in diagnosing a patient. However, in order to distinguish the type of liver lesion found on an ultrasound, more advanced imaging is usually necessary.
Learn more with our post on what to know about your liver ultrasound.
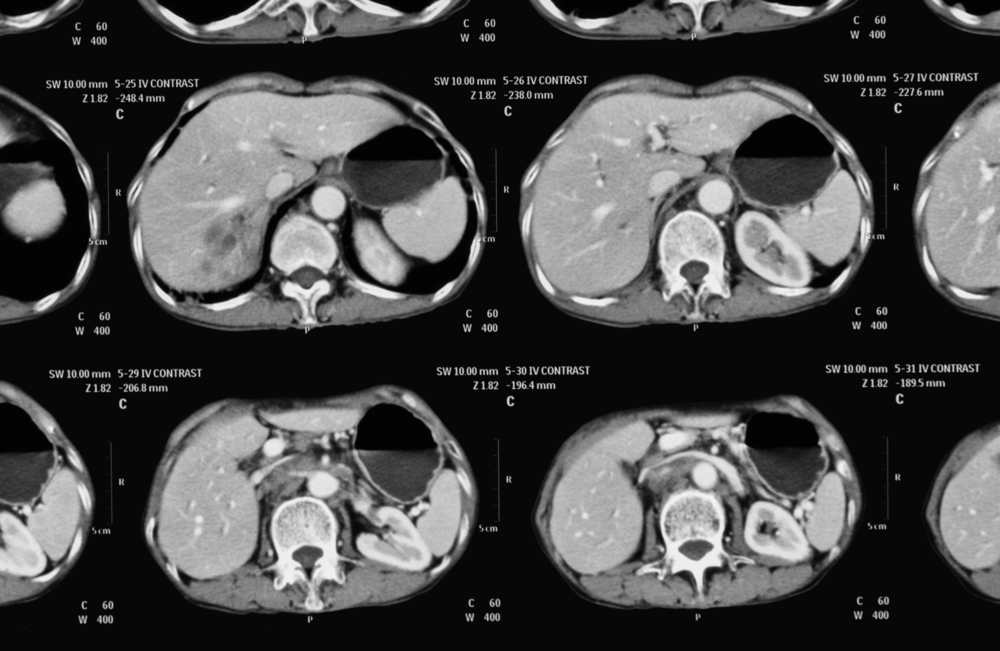
Liver Lesions on CT
A CT scan of the abdomen can help give specific information about the size, shape, and location of a mass in the liver. More advanced than an ultrasound, a CT provides a detailed approach to identifying the type of liver lesion. Intravenous iodinated contrast media are often used to further enhance the image. A CT-guided needle biopsy may also be used to test the malignancy of a tumor.
Liver Lesions on MRI
Like CT scans, MRI can be very helpful in differentiating liver lesions. It provides the most detailed look at soft tissue in the body and does not use ionizing radiation. MRI scans also offer high lesion-to-liver contrast – making it perhaps the most powerful imaging test for liver lesion detection. MRI can also be used to look at blood vessels in and around the liver.
According to leading expert in abdominal imaging, Dr Richard Semelka, “MRI with dynamic gadolinium imaging is the most powerful tool to evaluate the liver, but it also has the greatest requirement for skilled performance of the study and skilled interpretation of the studies. There is so much information available on an MRI, a radiologist must have a lot of training and experience in order to be very accomplished in interpreting all the findings.”
Liver Lesions on Angiography
Angiography involves injecting a contrast medium into an artery via a catheter. It’s used to outline blood vessels and can be helpful in identifying the arteries that supply blood to a liver cancer. However, it is relatively invasive. With the advances in CT and MRI contrasting, angiography is typically reserved as a last resort.
Get a Subspecialty Second Opinion Today
The DocPanel platform enables people all over the world to get an expert second opinion in as little as 24 – 72 hours.
An easy 3-step process – instantly upload your scans, select an expert subspecialty radiologist (or have DocPanel assign your case to the appropriate subspecialist), and submit your request. Upon uploading your scans, you’ll also have the opportunity to ask any questions you might have about your case. Not sure what a subspecialist is? Learn more with our in-depth article on the importance of getting a second opinion from a subspecialty radiologist.
This post has been medically approved by Dr. Richard Semelka. A lead expert in abdominal imaging, Dr. Semelka has been practicing radiology for over 28 years. He’s written over 16 text-books, 370 peer-reviewed papers, and has over 21,000 research citations in Abdominal Imaging.